Vision Benefits
Vision Plans
CSU Vision Plan - Basic
All eligible employees appointed half-time or more for a period of more than six months, and their eligible dependents, are automatically enrolled in the VSP Basic plan.
- Premiums are paid by the CSU.
- May visit any licensed ophthalmologist, optometrist or dispensing optician of choice.
- By choosing an in-network provider in the Vision Service Plan (VSP), the insurance may cover more out-of-pocket costs.
- Administrator is Vision Service Plan (VSP).
The VSP Basic plan includes:
- One comprehensive eye exam every calendar year.
- One pair of lenses every other calendar year (or calendar year if your prescription changes) and one frame every other calendar year.
- Contact lenses every other calendar year when contact lenses are provided in lieu of all other lenses and frame benefits.
Under VSP, the following vision benefits are available to eligible CSU employees:
- In-network frame allowance - $110
- Out-of-network frame allowance - $60
- In-network contact lens allowance - $120
- Discounts of approximately 15% for laser correction surgery are available
CSU Vision Plan - Premier
All CSU active employees eligible to participate in the CSU VSP Basic Plan are eligible to enroll in the Premier Vision Plan for a small monthly employee cost share. The Premier Vision Plan enables you to get a higher allowance for frames and contacts, fully covered standard progressive lenses, and more discounts.
The CSU will continue to contribute $7.10 towards the monthly premium which appears as a vision deduction on pay warrants. If the employee chooses the Premier Plan, the additional cost will be deducted directly from their pay warrant. Premier Plan will be administered by VSP.
If the employee elects the Premier Plan, any dependents they wish to cover must also be enrolled into the Premier Plan coverage. Employees cannot choose to enroll in both the Basic and Premier vision plan coverage at the same time, or split their enrollment leaving any dependents on the Basic Vision Plan. Eligible employees must enroll through VSP directly.
The VSP Premier plan includes:
- One comprehensive eye exam every calendar year.
- One pair of lenses/frames every calendar year.
- Contact lenses every calendar year when contact lenses are provided in lieu of all other lenses and frame benefits.
- Extra Savings on Retinal Screening.
Under the VSP Premier Plan, the following vision benefits are available to eligible CSU employees:
- In-network frame allowance - $210
- Costco/Sam's Club/Walmart frame allowance - $115
- In-network contact lens allowance - $200
- Polycarbonate lenses are covered for dependent children in-network up to age 23, instead of age 12
- Frames/lenses/contacts every calendar year
VSP Online Access
Employees can complete an online member registration enrollment to create a user identification (ID) and password, for the purpose of viewing his/her vision benefits at Active Employees | Retired Employees
The Consolidated Omnibus Budget Reconciliation Act (COBRA) - Vision
The Consolidated Omnibus Budget Reconciliation Act of 1986 (COBRA) and the Omnibus Budget Reconciliation Act of 1989 (OBRA) require employers to continue Medical, Dental, and Vision coverage for all eligible employees and dependents for up to 18, 29 or 36 months following certain events. The purpose of this continuation of coverage is to ensure access to health coverage for employees who would otherwise lose group coverage under specified circumstances called "qualifying events."
Employee Eligibility
An employee covered by a CSU health plan has a right to choose continuation coverage if group health coverage is lost because:
- Of a reduction in work hours; or
- The termination of employment (other than due to gross misconduct).
Spouse or Domestic Partner Eligibility
A spouse or domestic partner of an employee, covered by a CSU health plan, has the right to choose continuation coverage if group health coverage is lost for any of the following reasons:
- The death of the employee;
- Termination of employee's employment or reduction in employee’s work hours;
- Divorce, legal separation, or dissolution of domestic partnership from the employee; or
- Employee becomes entitled to Medicare.
Dependent Child Eligibility
A dependent child of a covered employee has the right to continuation coverage if group health coverage is lost for any of the following reasons:
- The death of the parent (employee);
- The termination of the parent's employment or reduction in the parent's work hours with the CSU;
- The parents' divorce, legal separation, or dissolution of domestic partnership;
- The parent (employee) becomes entitled to Medicare; or
- The dependent ceases to be a "dependent child" under the CSU health plan.
If an employee does not choose continuation coverage, the employee's coverage will end. However, the employee's spouse or domestic partner and/or eligible dependents may elect continuation coverage, independent of the employee's rejection.
COBRA coverage is effective from the date of the qualifying event. The CSU must notify eligible employees of their right to choose continuation coverage within fourteen (14) days of the qualifying event. An employee’s COBRA rights will be forfeited if the CSU does not receive notification of the employee’s wish to continue coverage within sixty (60) days of the qualifying event or date of the notification.
Following the sixty (60) day election period, an employee or eligible dependents have forty-five (45) days from the date of enrollment to pay for the continued coverage. The first payment will include the cost of coverage beginning with the first date coverage would have otherwise ended. After the initial payment, the required monthly premium is due before each month of coverage. Coverage will be cancelled if payment is not received within the thirty day grace period following each payment due date.
*COBRA premium rates are paid for by the participant. The CSU does not pay any portion of the COBRA premium. Please note, vision COBRA Rates are effective through December 31, 2023.
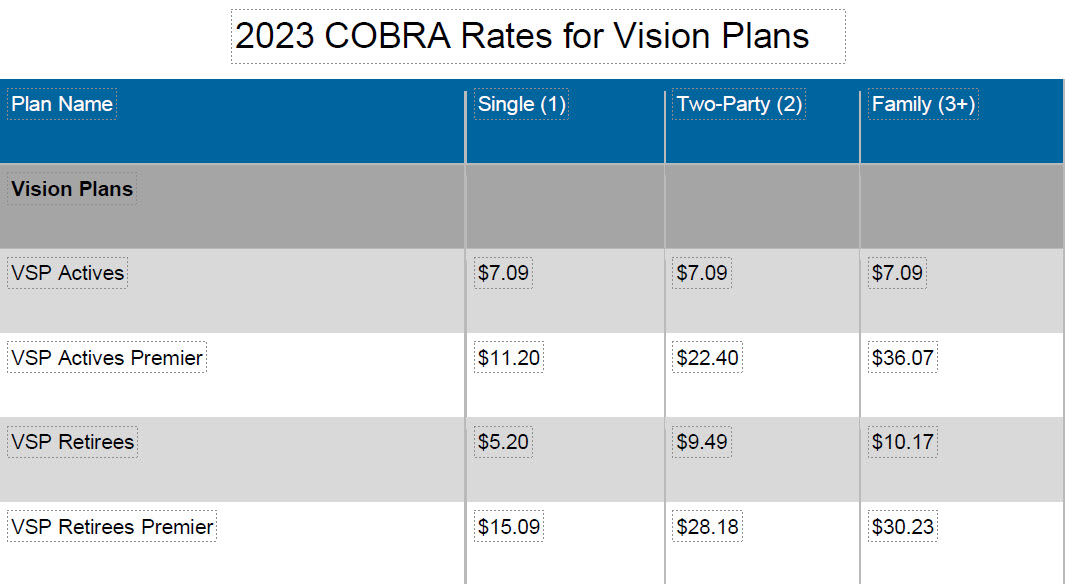
Vision
Vision Service Plan (VSP)
Phone: (800) 877-7195
Web site : www.vsp.com